I. Introduction
Glaucoma is a disease that causes blindness through the destruction of optic nerves. Glaucoma occurs because of a difficulty in producing and secreting the aqueous humor. It leads to irreversible vision loss.
Risk factors for glaucoma include age, family history, ethnic origin, diabetes mellitus, sex, elevated intraocular pressure (IOP), thin central corneal thickness, myopia, and hyperopia1).
In Korea, it was estimated that the prevalence of glaucoma in patients over 40 years of age increased from 0.79% in 2008 to 1.05% in 2013. The number of patients with glaucoma increased by 54% from 2008 to 2013. Costs associated with glaucoma care have also increased steadily2).
Age is one of the main risk factors for glaucoma3). Gupta & Chen reported the incidence rate of glaucoma for those aged over 80 and found that it ranged from 11.3% to 23.2% among black people; from 12.6% to 21.8% among Hispanics; and from 1.9% to 11.4% among white people in United States1). Because of the aging population in many countries of the world, adequate treatment and consistent follow-up on glaucoma are essential.
Generally, glaucoma is classified into two major subtypes: open-angle glaucoma and angle-closure glaucoma. The optic nerve degeneration of semiotic glaucoma appears in both types. Glaucoma can also be classified into the primary type and the secondary type. Secondary glaucoma occurs as a result of various pathologic risk factors, such as vasculopathy, malignancy, or trauma4).
Lowering the IOP is the best treatment for all kinds of glaucoma and its optic neuropathy5-8). The IOP is the only risk factor that can be controlled in glaucoma9). The main strategy to lower the IOP is medication (α-adrenergic agonist, β-blockers, carbonic anhydrase inhibitors, cholinergics, and prostaglandin analogues1)), although laser therapies or surgical therapies are possible alternatives. Surgical therapies, such as laser iridoplasty, trabeculoplasty, peripheral iridoplasty, and cyclophotocoagulation are sometimes needed to open the closed angle in angle-closure glaucoma10). The main treatment for congenital glaucoma is surgery, like goniotomy or trabeculotomy11-13).
In the present review, we evaluated recent studies on the effectiveness and safety of acupuncture therapy for glaucoma.
II. Methods
In this review, we followed the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines and the recommendations made by the Cochrane Collaboration (www.prisma-statement.org)14). The protocol of this review was registered in the International Prospective Register of Systematic Reviews, PROSPERO (CRD42018102801).
The following electronic databases were searched for relevant studies from their inception dates to September 1, 2018: the Cochrane Central Register of Controlled Trials (CENTRAL), EMBASE, MEDLINE, China National Knowledge Internet (CNKI), DataBase Periodical Information Academic (DB PIA), Korean Studies Information Service System (KISS), KMbase, KoreaMed, National Discovery for Science Leaders (NDSL), Oriental Medicine Advanced Searching Integrated System (OASIS), and Research Information Sharing Service (RISS).
The search terms used were “glaucoma”, “ocular hypertension”, “intraocular pressure”, “acupuncture”, “acupuncture therapy”, and “meridians”. The search strategies are described in Appendixes 1-11.
Randomized control trials (RCTs) designed to assess the effectiveness of acupuncture therapy for glaucoma were included. Other study designs, such as case reports, retrospective studies, and in vivo, in vitro studies, were excluded.
Patients with all types of glaucoma (open-angle glaucoma, angle-closure glaucoma, primary or secondary glaucoma, acute, subacute, or chronic glaucoma, and normal tension glaucoma) were included. Glaucomatous optic neuropathy caused by glaucoma was also included. There were no restrictions on age, gender, race, or region.
Acupuncture therapies to treat glaucoma were included. Acupuncture and electroacupuncture were selected as acupuncture therapies only. Other similar interventions, such as cupping, moxibustion, pricking blood, pharma-copuncture, and auricular acupuncture, which are classified as acupuncture therapy in a broad sense, were not included in this review.
Multiple interventions of Korean medicine, such as acupuncture combined with herbal medicine or pharmacopuncture were excluded. Acupuncture therapy alone or acupuncture therapy added to conventional therapy were included.
As a control intervention, a placebo, no treatment, and conventional therapies (medication, laser therapy, and surgical therapy) were considered eligible.
In this review, IOP, visual field (VF) loss and visual acuity(VA) are outcome measures.
An elevated IOP is the integral evidence for the primary diagnosis of glaucoma1). Consistent follow-up for IOP is very important to determine the progress and prognosis of glaucoma.
VF loss was selected as an outcome measure also. Visual damages due to glaucoma progress from the lateral vision to the central vision. Checking the VF is useful to evaluate the degree of progress of glaucoma as well as to assess the effectiveness of treatment15,16). There are Goldmann kinetic perimetry, Humphrey static perimetry, and Octopus static perimetry17-19). Kinetic perimetries are used to diagnose optic nerve pathway disorders, and static perimetries are used to evaluate the progress of glaucoma19).
The Humphrey filed analyzer (HFA) is easy to manipulate and is used worldwide because of its precise and reproducible results19,20). The HFA presents the results as a visual field index (VFI) and mean deviation (MD). The VFI presents visual function as a percentage, while the MD is an average of how much the VF test results are higher or lower than a normal VF21). The MD shows the severity of VF loss22) and the progress of glaucoma19). Therefore, it was selected as the measurement unit of VF loss in the present review.
The progression of glaucoma causes permanent blindness. Glaucoma patients are required to measure VA23,24). It has been reported that VA correlates with central vision sensitivity25). For that reason, VA was also adopted as an outcome measure in the present review.
After removing duplicates, the reviewer looked at titles and abstracts first. Then, the full texts of the selected randomized control trials that complied with the eligibility criteria were reviewed before the final selection of articles.
One researcher was in charge of extracting the data, while the other reviewed the extracted data. Data items extracted from each study were the author, published year, experiment site, sample size, patient age, gender, experimental and control intervention, outcome, acupuncture points, duration of treatments, frequency of treatments, and total session.
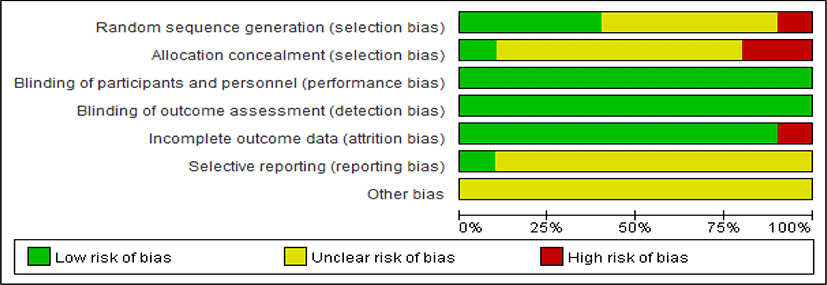
Two researchers assessed the quality of the research methodology by using the Risk of Bias (RoB) tool developed by Cochrane26). Each study was analyzed for the following six items: 1) selection bias (random sequence generation and allocation concealment); 2) performance bias (blinding of participants and personnel); 3) detection bias (blinding of outcome assessment); 4) attrition bias (incomplete outcome data reporting); 5) reporting bias (selective outcome reporting); and 6) other biases (baseline imbalance, other sources of risk). All included RCTs were categorized and graded as “high risk”, “unclear”, or “low risk”. Differences in the reviewers’ assessments were solved through a discussion with a third reviewer.
The meta-analysis and statistical analysis were conducted with RevMan (ver. 5.3) software by the Cochrane Collaboration. Because IOP, VF, and VA results, which were selected for outcome measures, are reported as continuous data, the weighted mean difference (WMD) or standardized mean difference (SMD) were used.
To estimate the heterogeneities, the chi-squared and Higgins I2 tests were adopted26). The Higgins I2 presents the percentage of the estimated value being caused by heterogeneity, not by chance.
If the I2 value is between 0% and 40%, the heterogeneity could be regarded as not important. From 30% to 60%, the heterogeneity is intermediate. An I2 value over 50% means substantial heterogeneity27).
The results of the chi-squared test have to be interpreted with caution because this test has a low statistical power when the size or the number of collected studies is small. Therefore, in the chi-squared test, the p-value uses 0.1 as the statistical significance level. If the p-value is over 0.10, the null hypothesis is accepted, and a fixed-effect model for meta-analysis is performed. If the p-value is under 0.10, the null hypothesis is rejected and the random effect model for meta-analysis is adopted27).
III. Results
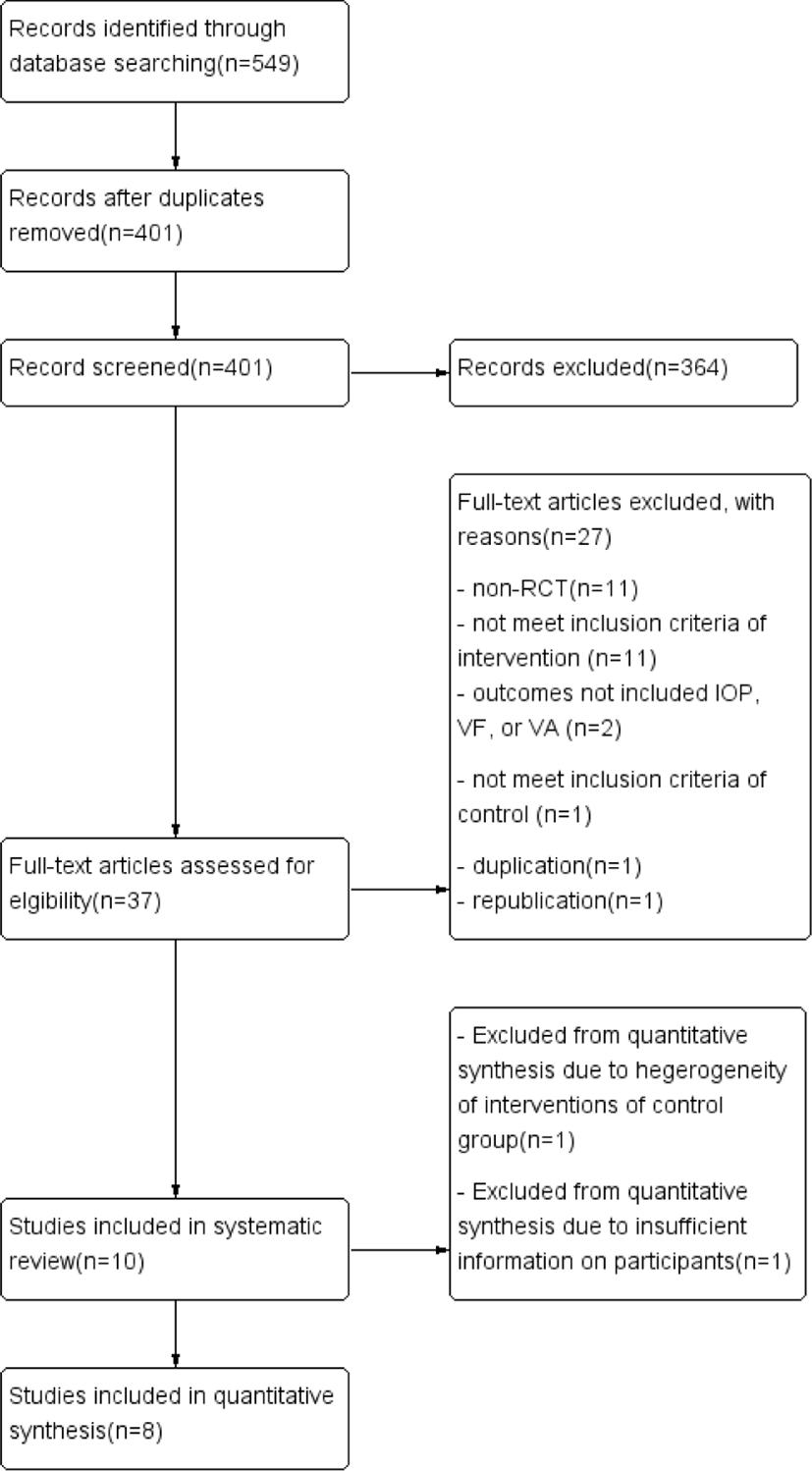
From the 11 electronic databases, 549 literature articles were initially retrieved; of these, 32 papers were extracted from CENTRAL, 13 from EMBASE, 18 from PubMed, 122 from CNKI, 138 from DB pia, 2 from KISS, 100 from KMbase, 32 from KoreaMed, 14 from NDSL, 42 from OASIS, and 36 from RISS.
After removing duplicates, a total of 401 studies remained. Of these, 364 studies were excluded after surveying their titles and abstracts. Full texts of 37 studies were reviewed and 27 studies were excluded because they were non-RCTs (11), used multi-interventions of Korean medicine like herbal medicine-acupuncture concurrent therapy or acupuncture-pharmacopuncture concurrent therapy (5), used a single intervention (e.g., pricking blood or pharmacopuncture) that was not regarded as acupuncture in this review (6), did not treat a control group with a conventional treatment, sham treatment, or no treatment (1), did not include the IOP, VF, or VA that are the outcome measures in this review (2), the study title was duplicated in two languages (Chinese and English) (1), or the study was republished (1).
Ten RCTs 28-37) were included in this systematic review and eight trials were selected for the final quantitative synthesis28-32, 34-36). One trial33) compared acupuncture with a placebo. Two trials29,35) compared only acupuncture therapy with conventional therapy. Six trials30-32,34,36,37) compared acupuncture and conventional concurrent therapy with conventional therapy (mainly medication using eye drops). One trial28) compared electro-acupuncture and conventional concurrent therapy with conventional therapy.
The IOP was adopted as an outcome measure in seven of the trials included in the quantitative synthesis28-32,34,35). VF was used as an outcome measure in four trials29,31,32,34) in the quantitative synthesis. VA was used as an outcome measure in three of the trials31,32,36) in the meta-analysis.
The entire process of screening and choosing articles is shown as a flow diagram in PRISMA (Fig. 1). The characteristics and outcomes of the 10 included studies are summarized in Table 1.
| First Author | Subtype of Glaucoma | Origination | Sample Size | Age(mean±SD) | Gender (M/F) | Experimental Intervention | Control Intervention | Outcome Measures | Duration | Frequency of Treatment | Total Session |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Zhang (2009)28) | §§POAG | China | 25/24 (43/43) |
48.49±3.52 | 21/28 | §EA+conventional therapy | Conventional therapy (timolol maleate) | 1) ∥IOP | 20min | daily §EA for 10 days a rest for 2 days repeat twice | 20 |
| Wu (2010)29) | §§POAG | China | 30/30 (60/60) |
(‡‡NR) | 33/27 | *AT | Conventional therapy (timolol maleate) | 1)∥IOP 2) †††VF(††N/A) 3) ***VA 4) ‡C value 5) †C/D ratio |
20-30 min | daily *AT for 10 days repeat 3 times | 30 |
| Liu (2013)30) | §§POAG | China | 10/9 (20/18) |
32.47±8.31 | 15/4 | *AT+conventional therapy | Conventional therapy (timolol maleate) | 1)∥IOP | 20min | daily *AT for 10 days a rest for 10 days repeat twice | 20 |
| Hao (2014)31) | glaucomatous optic neuropathy | China | 23/25 (44/45) |
57.57±12.62 | 18/29 | *AT+conventional therapy | Conventional therapy (medication that patients use) | 1)∥IOP 2) ¶MD 3) ***VA 4) ∥∥P-VEP 5) **MS |
30min | daily *AT for 14 days | 14 |
| Huang (2014)32) | §§POAG | China | 18/17 (29/29) |
44.3±7.1 | 17/18 | *AT+conventional therapy | Conventional therapy (timolol maleate) | 1) ∥IOP 2) ¶MD 3) ***VA 4) **MS |
20min | daily *AT for 10 days a rest for 2 days repeat twice | 20 |
| Law (2015)33) | §§POAG, glaucomatous optic neuropathy | United States | 11 (11/11) |
63.7±14.3 | 3/8 | *AT | *AT | 1) ∥IOP 2) ¶MD 3) ***VA 4) BP 5) HR 6) ¶¶RNFL 7) compiance 8) adverse reactions |
20min | 1-2 *AT per week | 12 |
| Sun (2015)34) | glaucomatous optic neuropathy) | China | 31/31 (60/54) |
54.8±3.08 | 25/37 | *AT+conventional therapy | Conventional therapy (carbonate dehydratase, β-Adrenergic antagonists, α-adrenoceptor agonists) | 1)∥IOP 2) †††VF 3) **MS |
30min | daily *AT for 2 weeks | 14 |
| Yang (2017)35) | §§POAG | China | 17/19 (26/24) |
>70 20people 50-69yrs 12people <50yrs 3people |
16/20 | *AT | Conventional therapy (timolol maleate) | 1)∥IOP 2) ¶MD |
30min | daily *AT for 7 days repeat twice | 14 |
| Wang (2017)36) | all | China | 25/23 (31/31) |
49.2±5.7 | 33/15 | *AT+conventional therapy | Conventional therapy (laser therapy, pranprofen, pilocarpine nitrate) | 1) ¶MD 2) ***VA 3) **MS |
‡‡NR | daily *AT for 12 days repeat 3 times | 36 |
| Wu (2018)37) | §§POAG | China | 28/30 (76) |
63.48±8.44 | 26/32 | *AT+conventional therapy | Conventional therapy (lanaprost) | 1) ∥IOP 2) ***VA |
30min | daily *AT for 10 days a rest for 1 week repeat 3 times | 30 |
*AT; Acupuncture Treatment; †C/D ratio; Cup to Disc ratio, ‡C value; coefficient value of outflow facility, §EA; electroacupuncture, ∥IOP; Intraocular Pressure, ¶MD; Mean Deviation, ** MS; Mean of Light sensitivity, ††N/A; Not Available, ‡‡NR; not recorded, §§POAG; Primary Open Angle Glaucoma, ∥∥P-VEP; pattern visual evoked potential, ¶¶RNFL; Retinal nerve fiber layer, ***VA; Visual Acuity, †††VF; Visual Field
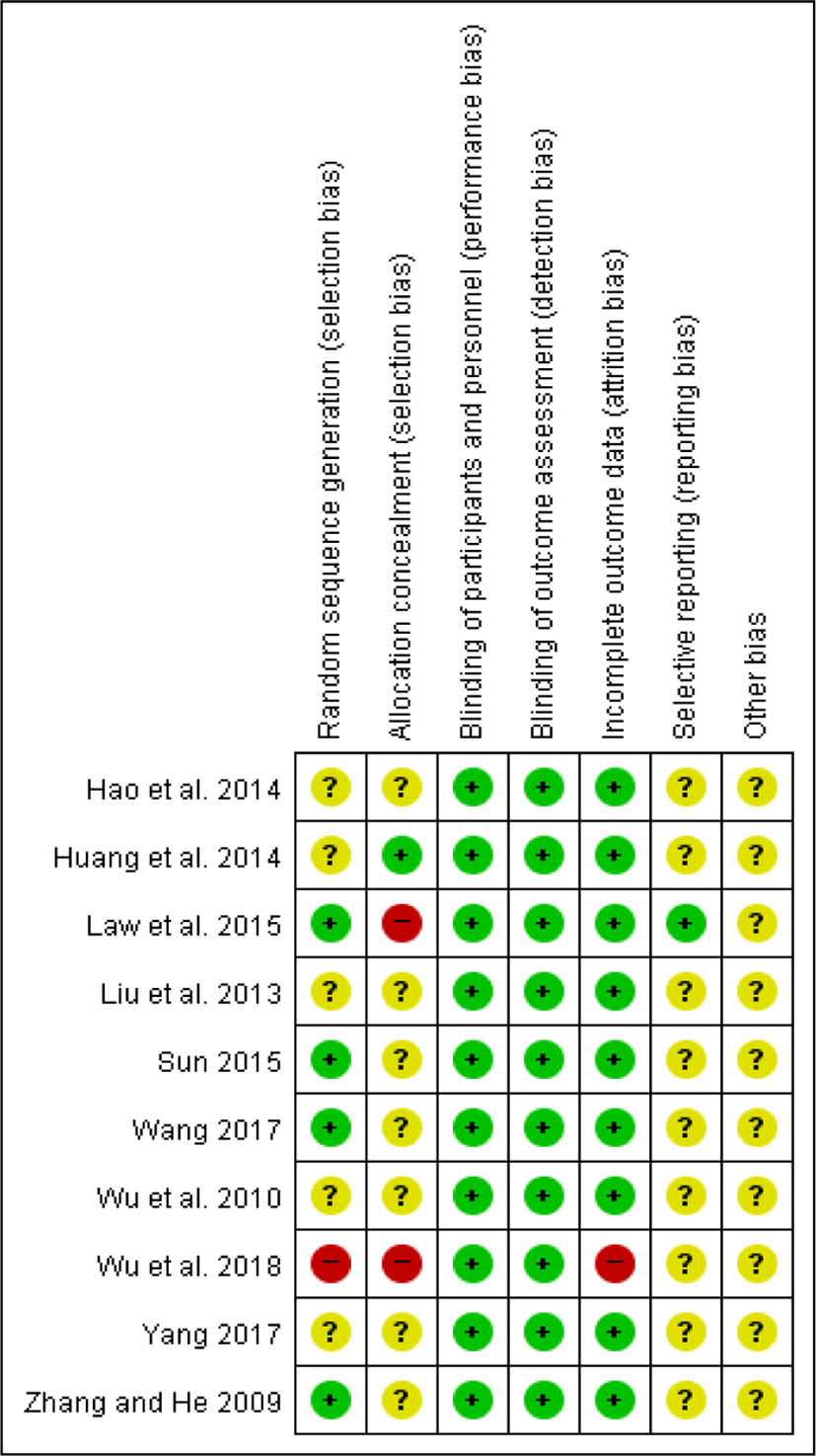
Among the 10 trials, four trials28,33,34,36) had a low risk of bias in the random sequence generation because they referred to how they managed the randomization. Five trials29-32,35) were assessed as an unclear risk of bias because they did not mention the method of randomization to divide the treatment group and the control group. One trial37) was assigned a high risk of bias because the authors randomized the treatment group and the control group in order of the patients’ arrival.
For allocation concealment, two trials33,37) were given a high risk of bias. In Law et al.’s trial33), patients who finished an acupuncture series (a treatment or sham treatment) were crossed over to receive the other acupuncture series. Wu et al.37) divided the treatment group and the control group in order of the patients’ arrival. It might provide a clue for investigators to assume whether a participant was assigned to the treatment group or to the control group. Eight trials28-31,34-36) were given an unclear risk of bias. Huang et al.32) reported that they chose a single-blind setup, but was given a low risk of bias because of the difficulty of a double-blind situation in the control group.
We requested more detailed information from the authors about the random sequence generation and allocation concealment from the researchers who provided their e-mail addresses in the respective papers (Hao et al.31), Yang35), and Wang36)), but did not get any response.
All included trials28-37) had a low risk of bias for the participants and personnel blinding. Law et al.’s trial33) was given a low risk of bias because they described that both the patients and research personnel (except the acupuncturists) were masked. In nine trials28-32,34-37), the experimental groups were treated independently with acupuncture or acupuncture and conventional concurrent therapy while the control groups were treated with conventional therapy. Although the blinding of the two groups was incomplete, but the outcome measures (IOP, VF, VA) of these trials were quantifiable and objective measures derived from the use of tools like tonometry, perimetry, and eidioptometry. In this respect, the outcomes were not likely to be influenced by a lack of blinding.
The reproducibility and accuracy of these outcome measures were assured by previous studies38), so all trials were given a low risk of bias for the blinding of outcome assessment. We supposed that the lack of blinding on the outcome assessors would not have been significantly affected.
With respect to incomplete outcome data, Wu et al.’s trial37) was assigned a high risk of bias because the authors did not offer sufficiently detailed information. They reported how many patients were involved in this experiment and divided them into the treatment group and the control group; however, they did not mention how many eyes of the patients were assigned in each group. We requested more information from the authors, but did not receive a response. This meant Wu’s trial37) could not be entered in the meta-analysis. The other nine studies were given a low risk of bias because they do not have missing outcome data28-30,32,34-36) or a reason for missing outcome data31,33).
Regarding selective reporting, one trial33) was given a low risk of bias because they described all expected outcomes. The remaining nine studies28-32, 34-37) were judged as an unclear risk of bias in selective reporting because there was insufficient information to permit judgement of a low or high risk of bias. We tried to contact the authors through their e-mail addresses in the respective reviews31,35-37) for more information, but did not receive a response.
For the other biases, we considered things like baseline imbalance or other sources of the risk of bias. All of the included trials were given an unclear risk of bias because they contained insufficient information to assess whether an important risk of bias exists or not(Fig. 2, 3).
Law et al.`s trial33) compared acupuncture therapy with a placebo. In this trial, patients received an acupuncture series with either eye-related or non-eye-related acupoints and then were crossed over to get the other series. After the individual treatment session, the average of IOP increased slightly with both eye-points (P=0.019) and non-eye-points (P=0.073). There were no significant differences in VF loss and best-corrected VA.
-
① IOP
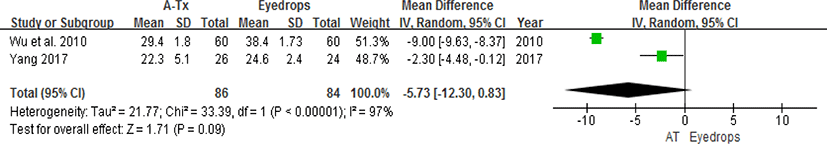
Wu et al.29) and Yang35) compared acupuncture therapy with conventional therapy (mainly eyedrops, medication). They used the IOP and VF as outcome measures. However, Wu et al.29) adopted kPa and Yang35) adopted mmHg as the measurement unit for the IOP. The units of the IOP in both studies were quantitatively synthesized in mmHg because kPa could be converted into mmHg39,40). The results of this analysis are as follows: WMD =-5.73, 95% CI: [-12.30, 0.83], P=0.09, I2 =97% (Fig. 4).
-
② VF
For the VF, the quantitative synthesis could not be performed because Wu et al.29) did not clarify which scale and unit they used to assess VF loss. Yang35) noted that they used the MD to evaluate VF loss.
There was no trial that did not adopt a treatment for the control group.
-
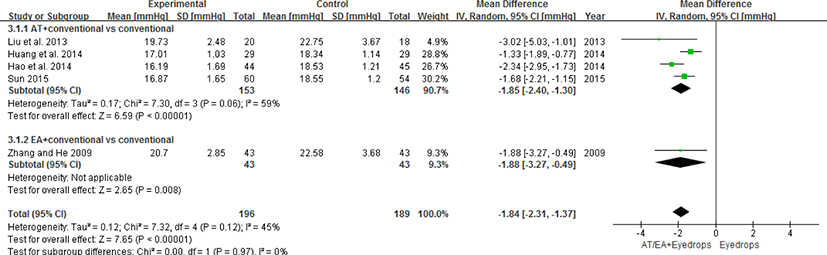
① IOP : Four trials30-32,34) compared acupuncture-conventional concurrent therapy with conventional therapy (eyedrops, medication). They adopted the IOP as an outcome measurement and used mmHg as the measurement unit of the IOP. After the meta-analysis, it is evident that acupuncture-conventional concurrent therapy is more effective to lower the IOP than conventional therapy alone (WMD=-1.85, 95% CI: [-2.40, -1.30], P < 0.00001, I2 = 59%) (Fig. 5).
One study28) compared electroacupuncture-conventional concurrent therapy with conventional therapy. The IOP was adopted as an outcome measure in this trial. The results suggest that electroacupuncture-conventional concurrent therapy is more effective than conventional therapy in lowering the IOP (electroacupuncture-conventional concurrent treatment group p<0.05, conventional treatment group p<0.05) (Fig. 5).
We synthesized these five RCTs28,30-32,34) that compared acupuncture/electroa-cupuncture combined with conventional therapy with only conventional therapy (mainly eyedrops, medication). The result of meta-analysis is as follows: WMD=-1.84, 95% CI: [-2.31, -1.37], P < 0.00001, I2 = 45% (see Fig. 5). The results demonstrate that acupuncture/electroacupuncture combined with conventional therapy is more effective in terms of lowering the IOP.
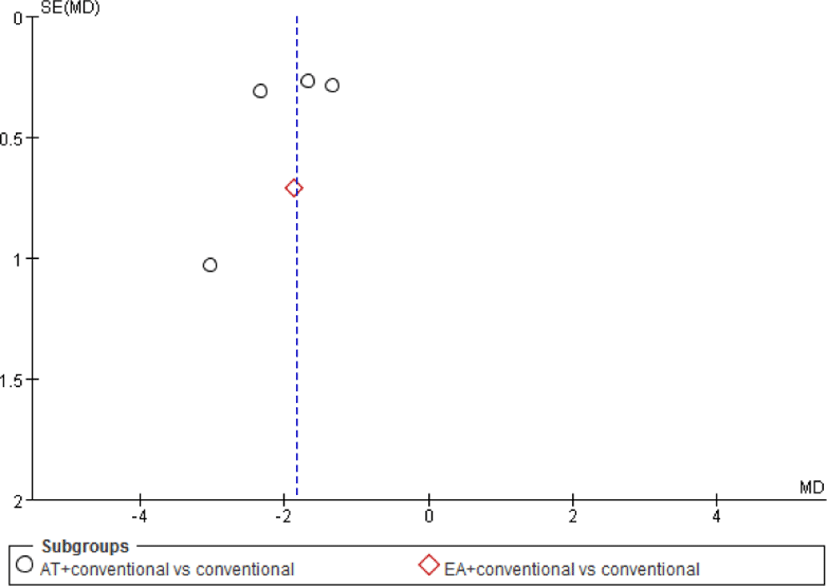
A funnel plot was created. A funnel plot is a scatter plot that visually represents public bias. It is expected that public bias would be small, since the funnel plot appears to be quite symmetric in this review. However, the funnel plot should be interpreted with caution, because the reviewed sample was not large (Fig. 6)41,42).
Wu et al.`s trial37) adopted acupuncture-conventional concurrent therapy and conventional therapy for both a treatment group and a control group, but was excluded due to insufficient information about the number of enrolled eyes. We requested more information from the authors via e-mail, but could not get a response.
-
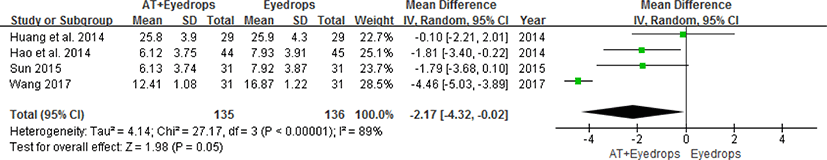
② VF : Four RCTs31,32,34,36) that used the VF as an outcome measure were analyzed to assess how much the VF was improved. Wang’s trial36) compared acupuncture-conventional concurrent therapy with conventional therapies (including medication and laser therapy). The trial was performed on the condition that the IOP was under control. All four RCTs31,32,34,36) used the MD that could be suggested by Humphrey perimetry. Because the MD is an output from the same diagnostic instrument, the outcomes were analyzed by WMD. The results of this analysis are as follows: WMD=-2.17, 95% CI: [-4.32, -0.02], P = 0.05 I2 = 89%. The results demonstrate that acupuncture-conventional concurrent therapy is more effective to improve VF loss than conventional therapy (Fig. 7).
-
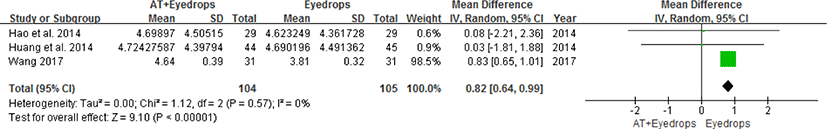
③ VA : To test the improvement of VA from acupuncture-conventional concurrent therapy, the results of three trials31,32,36) were synthesized. Two studies31,32) presented the VA value in decimal form and one study36) presented it in 5-logMAR. 5-logMAR is a way of stating VA values that is developed and used only in China43). Generally, converting logMAR to decimals or Snellen values at the group level is not recommended44). So, we transformed the decimal VA values into 5-logMAR and performed the meta-analysis. As a result, the effectiveness of acupuncture-conventional concurrent therapy was not confirmed statistically (WMD= 0.82, 95% CI: [0.64, 0.99], P<0.00001, I2 = 0%) (Fig. 8).
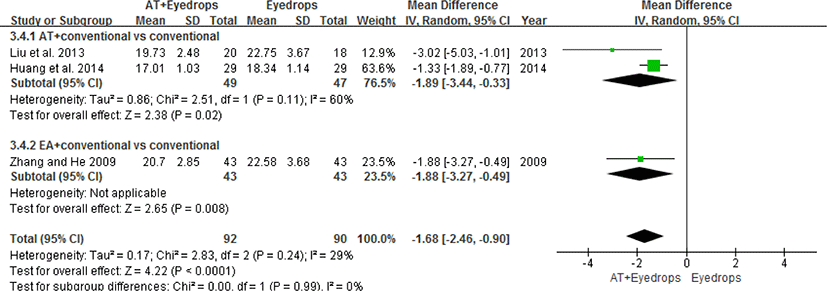
Three RCTs28,30,32) that treated the experimental group with electroacupuncture or acupuncture-conventional concurrent therapy studied primary open-angle glaucoma (POAG). Therefore, a subgroup analysis on the effectiveness of acupuncture for POAG was performed.
The results of the analysis of the three RCTs demonstrate that, regarding lowering the IOP, conventional therapy with acupuncture is more effective than conventional therapy alone (WMD=-1.68, 95% CI: [-2.46, -0.90], p<0.0001, I2 = 0%) (Fig. 9).
In the reviewed papers, we tried to find reporting of adverse events to prove the safety of acupuncture therapy.
One RCT33) recorded adverse events. An increase in the IOP in the fellow eye during acupuncture therapy was observed in one patient and two patients dropped out due to needle sensitivity.
Nine RCTs28-32,34-37) did not provide any information about adverse events (e.g., acupuncture syncope, hemorrhage, pain, infection, damage of organs, or any unexpected events) after acupuncture therapy. Acupuncture therapy seemed not to cause serious adverse events, but the evidence is limited.
IV. Discussion
This study was conducted to evaluate the effectiveness and safety of acupuncture therapy for glaucoma. The pooled results indicated that acupuncture reduced the IOP significantly when it was used independently or combined with conventional therapy. Acupuncture-conventional concurrent therapy was more effective than the conventional therapy alone in improving VF loss also. We could not find any evidence that acupuncture therapy is effective in improving VA. Acupuncture/electroacupuncture combined with conventional therapy appears to be more effective in lowering the IOP than conventional therapy in the treatment of POAG. The results of systematic reviews and meta-analysis showed the benefit of acupuncture for glaucoma. But these results need to be interpreted cautiously due to the methodological inconsistencies and heterogeneities of the data.
Acupuncture therapy involves stimulating specific regions of the body with acupuncture needles to promote positive effects on health45). It is reported that acupuncture therapy might provoke somatoautomic reflexes and have some positive effects for homeostasis22). Previous research has also demonstrated that acupuncture and electroacupuncture could activate neural pathways, both central and peripheral, and adjust the secretion of neurotransmitters46). Acupuncture treatments might also have a positive impact on the neuroendocrine system47,48).
Dai et al. conducted a meta-analysis aimed at assessing the effectiveness of acupuncture for optic atrophy49). According to the results of this study, concurrent acupuncture-medication therapy could improve one’s VF and VA. Likewise, the American Academy of Ophthalmology’s task force also acknowledged that acupuncture therapy may be both a valuable and adequate alternative to conventional therapies50).
The IOP is the most dangerous and the only adjustable risk factor for glaucoma5,7,51,52). As the IOP increases, glaucomatous optic nerve destruction is aggravated7). Therefore, controlling the IOP to prevent destructive or functional degeneration of optic nerve is the primary treatment. In addition, finding various treatment approaches to lower the IOP is very important.
In the present review, the acupoints EX-HN528,30-32,34-37) and BL128,30-32,34-37) were adopted in seven studies. GB2028,31,34,36,37), LR330,32,33,35,37) and LI431,33-35,37) were referred to five times, and GB3728,30,33,37), ST131,34-36) and BL228,33,36,37) four times. EX-HN5, BL1, BL2, GB20, ST1 are proximal acupoints, while LR3, LI4 and GB37 are acupoints on extremities. Acupoints were represented by the World Health Organization Standard on Acupuncture Point Locations in the Western Pacific Region53). Seven studies recorded they did twirling manipulations very mildly or did not do that, especially on eye-related acupoints29-32,34,36,37).
The results of the present review demonstrated that both acupuncture and electroacupuncture are useful for lowering the IOP. Therefore, adding acupuncture or electroacupuncture to conventional therapies (mainly medication) would be helpful to decrease the IOP and thus to improve the condition of glaucoma patients. Also, our results suggest that acupuncture can improve the VF; however, further research is needed on this issue due to the small size of the sample in our review.
Previous systematic reviews sought to examine the effectiveness of acupuncture for glaucoma. For instance, Gao et al.54) collected eight RCTs and quantitatively analyzed four of them. However, the definition of intervention used in that study was too broad. Specifically, pricking blood, acupuncture, and electroacupuncture were regarded as the same intervention.
Pricking blood is one of the acupuncture and moxibustion therapies that came from the ‘Yellow Emperor’s classic of Internal medicine’55,56). Pricking blood involves bleeding a patient from the extremities or in a strained region to relieve tensions and pain. Pricking blood helps to adjust blood pressure and an imbalance of the autonomic nervous system45,57). Pricking blood is a kind of an acupuncture therapy, but differs from acupuncture or electroacupuncture because it must make patients bleed. As interventions used in the reviewed studies were diverse, the heterogeneity could differ considerably.
Law & Li58)conducted a systematic review in 2013, but could not quantify the magnitude of the effect. The present review contributes to the available literature by complementing the previous reviews and by using more precise selection criteria and definitions (e.g., that of intervention). And this review is the largest-scale study among existing studies on this issue. Additionally, we used the VF and VA as outcome measurements.
The strengths for this review are as follows. Comprehensive searching through databases in various languages was conducted to identify every relevant article. Interventions were categorized in detail and many attempts have been made to confirm the effectiveness of acupuncture on multiple symptoms of glaucoma such as an elevated IOP, VF loss, and VA loss.
Yet the sample size used in the present review was rather small and the methodological qualities of some studies were low, which could lead to an overestimation of the effects of acupuncture on glaucoma. We contacted the authors to get more information about their methodologies, but did not get any response.
There were significant heterogeneities in some outcomes even though a classification of interventions was conducted. Thus, it is difficult to draw definite conclusions on the clinical effectiveness of acupuncture for glaucoma. Most of included studies were conducted in China, which may suggest the potential for a location bias.
To improve the quality of the research method used in the present review, it is recommended that a new study chooses RCTs that employ rigorous randomization methods and blinding procedures. Future studies need to provide sufficient descriptions of their samples and research procedures. Furthermore, larger-scale reviews, including the results coming from different countries, should be undertaken in the future. In addition, studies comparing acupuncture therapy with sham therapy need to be conducted more. There was only one study which was comparing acupuncture therapy with sham treatment. And there was no trial that did not adopt a treatment for the control group. This is needed to be investigated more also. Finally, adverse events also need to be properly and adequately assessed and reported for assuring the safety of acupuncture.
V. Conclusions
According to the results of the present systematic review and meta-analysis, acupuncture therapy alone could reduce the IOP more than conventional therapy. When acupuncture or electroacupuncture therapy was used with conventional therapy concurrently, it was more effective in lowering the IOP than conventional therapy. Acupuncture-conventional concurrent therapy could also lessen VF loss. For POAG, acupuncture therapy combined with conventional therapy appears to be more effective in lowering the IOP than conventional therapy.
However, due to the limitations of this review, further research needs to use rigorous research designs and larger sample sizes from various countries.